Pelvic floor dysfunction affects millions of people worldwide, causing discomfort, incontinence, and a reduced quality of life. Pelvic floor repair is a specialized treatment designed to restore the strength and function of the pelvic muscles, supporting the bladder, uterus, and bowel. Whether caused by childbirth, aging, or chronic strain, effective repair can significantly improve daily life, confidence, and overall health.
Understanding Pelvic Floor Dysfunction
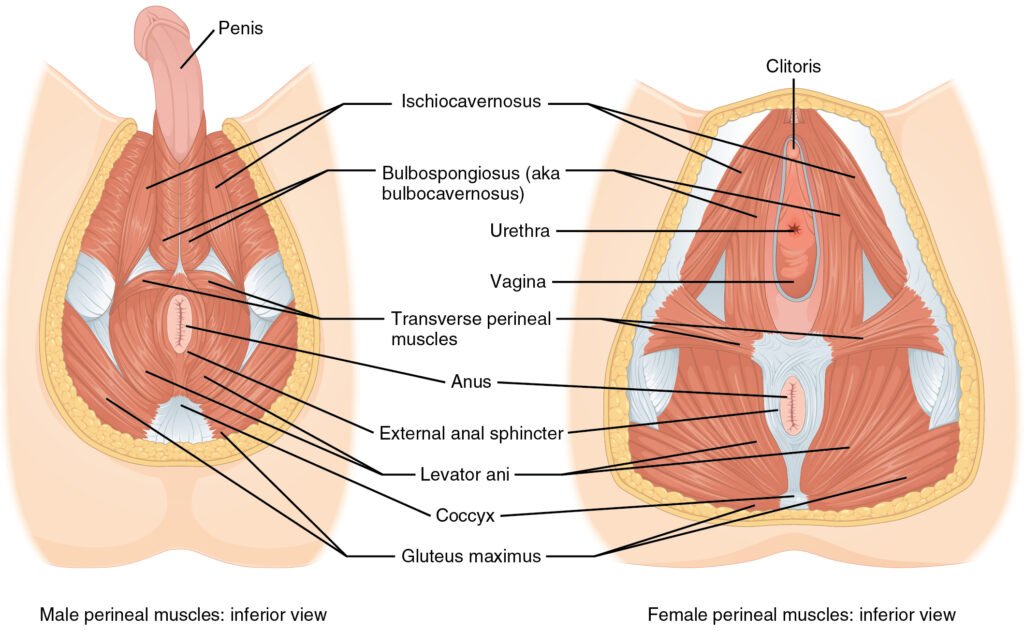
The pelvic floor is a group of muscles and connective tissues that form a supportive hammock for pelvic organs. When these muscles weaken, stretch, or tear, issues like urinary incontinence, pelvic organ prolapse, and sexual dysfunction can occur. Symptoms may include:
- Difficulty controlling bladder or bowel movements
- Pelvic pain or pressure
- Discomfort during sexual activity
- Lower back or hip pain
Identifying symptoms early is crucial for successful treatment and recovery.
Pelvic Floor Repair Procedures
Pelvic floor repair can be surgical or non-surgical, depending on severity and patient needs.
1. Non-Surgical Approaches
- Pelvic Floor Physiotherapy: Targeted exercises such as Kegels strengthen muscles and improve control.
- Biofeedback Therapy: Uses sensors to teach patients how to engage pelvic muscles effectively.
- Vaginal Devices or Pessaries: Support prolapsed organs and reduce pressure.
2. Surgical Repair
For severe cases like significant prolapse or muscle tearing, surgical intervention may be necessary. Procedures include:
- Anterior and Posterior Repair: Strengthening the front or back walls of the vagina to correct prolapse.
- Sacrocolpopexy: Attaching pelvic organs to the sacrum for long-term support.
- Minimally Invasive Laparoscopic Surgery: Offers faster recovery and less discomfort.
The choice of procedure depends on the type and severity of dysfunction, patient health, and the surgeon’s recommendation.
Recovery and Rehabilitation
Post-repair recovery is crucial for long-term success. Recovery tips include:
- Rest and Limited Strain: Avoid heavy lifting and high-impact activities for several weeks.
- Pelvic Floor Exercises: Gradually reintroduce exercises to strengthen muscles after medical clearance.
- Pain Management: Follow prescribed medications and attend follow-up appointments to monitor healing.
- Lifestyle Adjustments: Maintain a healthy weight, manage constipation, and avoid activities that increase pelvic pressure.
Recovery time varies depending on the procedure, typically ranging from 4–12 weeks. Patients who follow rehabilitation guidelines often experience improved muscle tone, reduced prolapse symptoms, and enhanced sexual health.
Benefits of Pelvic Floor Repair
- Restores bladder, bowel, and sexual function
- Reduces discomfort and pelvic pressure
- Improves confidence and quality of life
- Prevents further complications
Choosing the Right Specialist
Selecting a qualified gynecologist, urogynecologist, or pelvic floor surgeon is vital. Look for professionals experienced in both surgical and non-surgical techniques, with a comprehensive approach to patient care. Clinics in major hubs like Dubai often provide advanced treatments, combining expertise with state-of-the-art technology.
Many clinics also address related conditions, such as vaginal dryness solution Dubai, which often coexists with pelvic floor dysfunction. Addressing both issues together can significantly enhance comfort, sexual health, and recovery outcomes.
Final Thoughts
Effective pelvic floor repair offers life-changing results for those struggling with dysfunction. Whether through targeted exercises, minimally invasive surgery, or a combination of approaches, patients can regain control, reduce discomfort, and improve overall well-being. Consulting a qualified specialist and following a structured rehabilitation plan ensures the best possible outcome and long-term pelvic health.